Lessons from Farzad Mostashari, CEO and Co-Founder of Aledade, on Empowering Independent Primary & Value-Based Care
Farzad Mostashari, CEO and Co-founder of Aledade, an organization that helps independent primary care practices succeed in a physician-led ACO.
Subscribe to our substack for weekly updates and listen on Apple Podcasts or Spotify. Connect with me if you find this post insightful and want to learn more.
Welcome back to the Pear Healthcare Playbook! Every week, we’ll be getting to know trailblazing healthcare leaders and dive into building a digital health business from 0 to 1.
Today we're excited to get to know Dr. Farzad Mostashari, CEO and Co-founder of Aledade, a primary care enablement company that partners with independent PCPs to transition to value-based care. Founded in 2014, Aledade works with over 11,000 physicians across 40 States accounting for 1.7 million patients under management in Medicare, Medicare Advantage, commercial, and Medicaid contracts.
Farzad has spent his career in health care policy and health information technology.
Farzad previously served as the National Coordinator for Health IT in the Department of Health and Human Services. Prior to his work at the Office of the National Coordinator, he founded the NYC Primary Care Information project, which equipped physicians and underserved communities with electronic health records. He completed medical school at the Yale School of Medicine and a Master’s degree in Population Health from Harvard’s T.H. Chan School of Public Health.
In this episode we talk about Farzad’s journey to healthcare, how he started Aledade, the importance of independent physicians in value-based care, how Aledade scaled as a profitable health tech company, and advice he has for founders.
If you prefer listening, here’s the link to the podcast!
What Drew Farzad to Medicine & Public Health
In the realm of healthcare, there are those whose calling is driven by a desire to give back, to make a tangible difference in the lives of others. Farzad embodies this ethos especially with his passion for public health.
His journey to medicine was sparked when his father fell ill and required hospitalization. It was during this critical period when an interest in medicine emerged, but his passion for public health never waned; it became an indelible presence, quietly shaping his journey.
Dr. Mostashari describes himself as someone who never quite felt like an insider, despite his affiliation with esteemed institutions in the American healthcare system. He constantly straddled the worlds of public health and medicine
"I always felt a little bit of an outsider. When I was in public health, I constantly thought about medicine, and when I was in medicine, I consistently thought about public health. I have been living in those boundary areas, tirelessly striving to bring those two fields closer together."
Farzad's education in public health equipped him with the necessary tools to think critically and challenge prevailing assumptions. His studies in epidemiology and research design provided him with the means to navigate the complex landscape of population and public health. By adhering to evidence-based practices, he was able to eliminate reliance on unreliable anecdotes and subjective assessments.
“You can't trust what you think probably works, you really have to design the work in a way that can yield generalizable information about what works and what doesn't work in Population and Public Health”
The Digitization of Public Health and Healthcare
In the late 1990s, during the rise of the internet and the digitization of various sectors, Farzad embarked on his first post-fellowship role: launching the Bureau of Epidemiology Services at the NY City Health Department. This was an era when medical records were predominantly paper-based, but billing systems had started to transition to electronic formats.
“Patients would come into the emergency room and even though the medical records were on paper, the billing systems were electronic. When someone bought medicine at the pharmacy and it got scanned at checkout, that transaction created real-time data. With all this digital data across the computer, I got interested if we could use that for public health surveillance, which was called syndromic surveillance at the time.”
Syndromic surveillance involved the collection of health-related data as early as possible when illnesses surfaced, enabling a comprehensive understanding of disease spread within the population. It required a collaborative effort among computational experts, emergency room doctors, public health professionals, and epidemiologists to leverage real-time digital data for monitoring and public health surveillance.
“I was tasked by my boss Tom Frieden and his boss Mike Bloomberg, former Mayor of New York city, to figure out how to save the most lives in NY city. We took a data driven approach, which led us to prioritizing smoking cessation in NY city.
Their comprehensive tobacco control plan included measures such as increased cigarette excise taxes, legal actions to establish smoke-free workplaces, and enhanced smoking cessation services. These combined efforts resulted in a remarkable 11% reduction in smoking rates, equivalent to 140,000 fewer smokers, between 2002 and 2003.
While these initiatives successfully addressed a public health concern, the issue of prioritizing healthcare interventions to save lives still lingered. With a staggering $4.2 trillion spent on medical care in the United States, insufficient attention had been given to determining which interventions could have the greatest impact. The answer became clear: controlling blood pressure. Astonishingly, over 122 million Americans suffer from high blood pressure, making it a pressing matter to address
“We took a data driven approach similar to smoking cessation and tried to digitize American Healthcare as a way to save the most lives by controlling blood pressure. I spent the next 10 years in charge of programs and policies to try to get electronic health records into clinical offices and hospitals.”
Despite these efforts, blood pressure control actually worsened over the past decade. The digital transformation alone was not to blame for this setback; rather, it failed to provide an all-encompassing solution for the issue.
Farzad realized that financial incentives played a crucial role in the equation. In a fee-for-service payment system, the emphasis lies on treatment rather than prevention. Consequently, investments are directed towards managing stroke, kidney failure, heart attacks, and other conditions, perpetuating a reactionary approach to healthcare. Regrettably, the health system, at the time, did not adequately reward preventive measures such as blood pressure control.
The Start of Aledade
At the New York City Department of Health, Farzad and his colleague Mat Kendall collaborated on the Primary Care Information Project, an initiative aimed at implementing electronic health records in physician practices. Their collaboration continued as they worked together on implementing the HITECH Act at the Office of the National Coordinator of Health IT in the Department of Health and Human Services, where Farzad eventually assumed the role of National Coordinator.
As the Coordinator for Health Information Technology, Farzad played a crucial role in driving the adoption of electronic health records (EHR). Under his leadership, EHR adoption rates soared from 9% to an impressive 90%. Moreover, Farzad along with other agents were instrumental in setting the criteria that EHR companies needed to meet in order to receive payments.
However, a significant challenge arose. While there was substantial power to enforce compliance, there was a lack of emphasis on improving outcomes or incentivizing positive changes.
“We’re not looking for this to be a box checking exercise to enforce compliance with EHR companies in order to get paid. We wanted it to be an ongoing business model where an organization makes profits by controlling blood pressure instead of just merely implementing a system that has blood pressure decision support.”
The focus needed to shift from compliance to outcomes-driven incentives.
Initially, Farzad attempted to secure a government-funded approach to facilitate this transformation. However, realizing the unlikelihood of this approach, he recognized the need for an entrepreneurial effort from the outside.
“It all started with the goal of getting as many patients served under a new payment and delivery model that incentivizes prevention and saves the most lives. Do you work with hospitals, health systems, or nonprofits? Or do you go upstream and to primary care. The clear answer was to go upstream and prioritize primary care.”
With this in mind, the focus of the business model of Aledade centered on partnering with independent primary care clinics for scalability and reduced capital intensity, as opposed to building new primary care clinics or collaborating exclusively with hospital-affiliated primary care clinics.
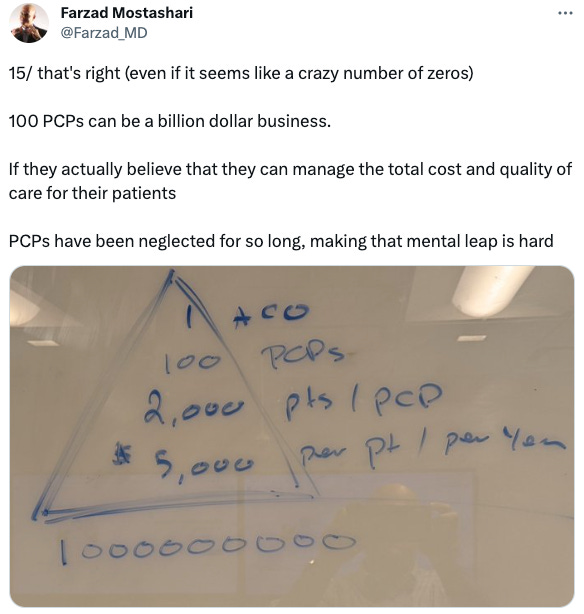
This brought accountable care organizations (ACOs) into the picture, as they presented an opportunity to combine financial incentives with technology investments. Aledade was founded on this premise along with the idea that a network of 100 PCPs can be a billion dollar business.
The average primary care physician has a panel of 2000 patients, each of whom incurs roughly $5,000 in annual medical costs. This implies that a network of just 100 PCPs manages patients accounting for $1B of healthcare spend.
“Our strategy aligns with the fundamental assumptions and ideas underlying our mission. By taking accountability for the total cost and quality of care for a population, and by actively working to reduce hospitalizations and adverse events, we create savings that we can distribute. This is the essence of value-based care”
Aledade, along with primary care companies like Oak Street Health and Chenmed, shares a core mission of shouldering the burden of total cost of care risk and striving to lower healthcare expenditures for revenue generation. However, they diverge in terms of their operational and business approaches. Aledade, unlike its counterparts, does not focus on constructing or acquiring practices; instead, it forges partnerships with existing independent physician practices that are not affiliated with health systems.
In many industries, consolidation often leads to improved quality and lower costs. However, the healthcare sector does not always follow this trend. In fact, healthcare consolidation often results in limited choices, higher costs, and poorer quality of care. This is precisely why Aledade is placing its bets on independent primary care practices, recognizing their potential to deliver superior outcomes and a more patient-centered experience when it comes to value-based care.
Policy Makers as Part of the Core Team
When Farzad initially assembled his team for Aledade, he brought together an exceptional group of individuals who possessed deep expertise in public policy but had been undervalued by the market.
“Healthcare is a highly regulated environment, so people with experience in healthcare and public policy expertise have incredible knowledge of healthcare, are mission-driven, and are incredibly competent, and you can get them at fraction of the price you would have to pay for someone coming out of Harvard Business School because they are used to government salaries”
In the early stages of Aledade's growth, many of the team members were drawn from public service backgrounds. As the company expanded, they began incorporating individuals with diverse business experiences, including several individuals from renowned organizations such as Tesla, Google, and Meta.
“For aspiring founders, you always need to think about the assets you have. This can include something you know that other people don’t know. In my case, it was recognizing the exceptional qualities of public servants!”
Public policy and regulations can often be seen as a potential risk for startups operating in specific industries. However, having individuals well-versed in those areas can actually present as an opportunity.
While public policy and regulations may appear as potential risks for startups in specific industries, Farzad points out that having individuals well-versed in these areas can actually present opportunities. Aledade's journey began during the initial phase of the Medicare Shared Savings Program (MSSP). They realized that the program's original design was flawed, particularly in accurately calculating savings. Leveraging their experience as policymakers, they foresaw the program's inevitable changes aimed at enhancing its effectiveness. When these changes occurred, people were curious about how Aledade seemed to possess advanced knowledge.
“It wasn’t rocket science. You start with the assumption that the regulators know a lot, and want to do the right thing for America, then build your business such that if they did the right thing, you would benefit.”
One specific policy change revolved around the concept of a counterfactual in benchmarking within the MSSP. Initially, the program determined benchmarks by using the previous year's costs, posing a problem because reducing costs would simultaneously lower benchmarks.
However, after a few years, CMS decided to divide the benchmark into two parts: historical and market average. Essentially, half of the benchmark was based on the individual organization's performance, while the other half was derived from competitive averages. Aledade foresaw this policy change and successfully assisted primary care physicians (PCPs) and accountable care organizations (ACOs) in achieving significant cost savings.
Aledade specifically helps PCPs and ACOs achieve these cost savings through its 4 core competencies below:
A 2-sided marketplace for Aledade
Aledade approached the Medicare Shared Savings Program (MSSP) by strategically considering the interplay between new payment models and delivery systems. The team recognized the need for consolidation among multiple payer contracts and the importance of creating a substantial risk pool that would allow them to take calculated risks.
"Instead of going through an application process and engaging in extensive negotiations with different payers, the MSSP program provided us with a unique opportunity. With a single move, we could enroll all the traditional Medicare patients, which served as our anchor tenant and enabled us to achieve critical mass."
Once Aledade had successfully enrolled enough practices under the MSSP program, they had accumulated a sufficient number of patient lives. Armed with this substantial patient population, they were then able to approach payers and negotiate contracts.
“When we already have 5,000 or 10,000 members within our practices, obtaining contracts from payers becomes easier. In some cases, we took a different approach and positioned ourselves to the commercial side by highlighting our existing connections such as Blue Cross, Medicare, and Medicaid contracts.”
This process sets in motion a mutually reinforcing cycle. The more practices Aledade accumulates, the more leverage they have in securing health plan contracts, and vice versa. Aledade's success is exemplified by their extensive portfolio of hundreds of different health plan contracts, each obtained with greater ease compared to their initial endeavor.
Future of Aledade
Aledade has recently achieved a significant milestone by raising a substantial $260 million in a Series F funding round, led by Lightspeed Ventures, increasing Aledade’s valuation.
However, Farzad emphasizes that founders should never mistake valuation as the sole guiding metric.
“Never confuse your valuation with your value. Market dynamics can sometimes cause our valuation to be ahead of or behind the value we're actually creating. Instead of fixating on valuation, you and your team should focus on the tangible outcomes you're bringing about. For us, it's about the number of hospitalizations we've prevented and the amount of savings we've been able to return to providers”
Launching new practices and building interfaces follows a J curve pattern, where significant upfront costs are incurred, and it takes a couple of years for a practice to become profitable. Therefore, many healthcare companies, including Aledade, need to raise funds to facilitate growth and enhance their product offerings.
“We have to invest constantly in more innovation and technology to make it easier for practices to follow through on their commitments and their patients. Last year we launched Aledade Care Solutions, which basically creates a way to get warm handoffs from primary care to wraparound solutions. We also acquired Iris Healthcare, a comprehensive advanced care planning for end of life decision making.”
Iris Healthcare, through its virtual Comprehensive Advance Care Planning services, strengthens the trusted relationship between physicians and patients, providing clarity on values and care preferences for complex medical conditions.
In a randomized study conducted alongside Aledade, Iris Healthcare demonstrated a remarkable Net Promoter Score (NPS) of 92 and achieved additional cost reductions ranging from $4,000 to $10,000.
The secured funding will empower Aledade to seek out mission-aligned companies that deliver exceptional solutions to patients and practices, further advancing Aledade’s goals.
Advice for Founders
Entrepreneurs in the healthcare industry have a tremendous opportunity to create specialized services catering to specific patient populations, such as kidney care, cancer, and various other areas. This opportunity is particularly significant with the CMS goal of 100% original Medicare beneficiaries and the majority of Medicaid in accountable care by 2030.
It is crucial to subject your businesses and companies to rigorous stress tests in various ways. If your company can withstand a randomized clinical trial and demonstrate significant positive effects on a patient population, it holds tremendous power.
Rather than placing emphasis on marketing strategies, patient outreach, or Net Promoter Scores (NPS), it is imperative to evaluate the primary measure of success for your business. The key consideration should be centered around assuming full accountability for outcomes. By shifting the focus away from valuation, you and your team should prioritize the tangible and measurable outcomes that you have the potential to achieve.
Thanks for reading Pear Healthcare Playbook! Subscribe for free to receive new posts and support my work.
Interested in Aledade or joining their team? Learn more on their website, Twitter, and LinkedIn
A note from our sponsor: PacWest
Looking for guidance, connections, resources, opportunity? Pacific Western Bank’s banking products and services are built to support your evolving needs as you navigate the challenges of growing a successful business. As you continue to scale, our team will be with you every step of the way. Ready to take your business to the next level? Learn more: pacwest.com